
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|


Are You Prepared
to Restrain an Agitated Patient?
*FACTS:to Restrain an Agitated Patient?
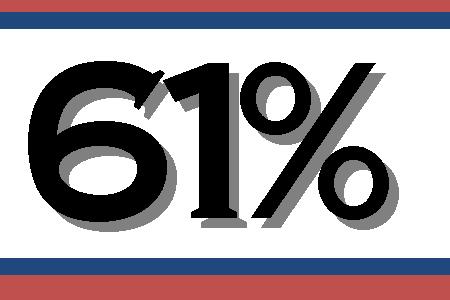
Percentage of EMS providers who reported having been assaulted on the job,
with 25% of those reporting injury. Of those injured, 37% required medical attention.
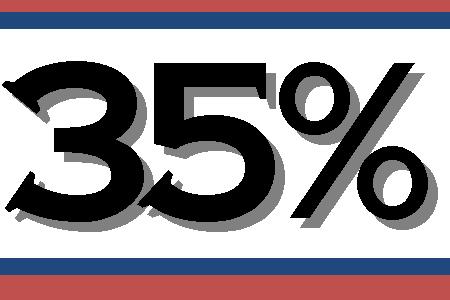
Percentage of EMS providers working for a provider that had
specific protocols for management of combative and/or violent patients.
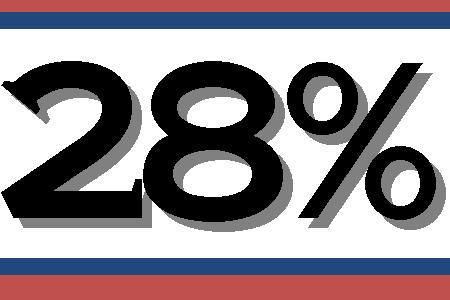
Percentage of EMS providers reported having received
any formal training on pre-hospital patient restraints.
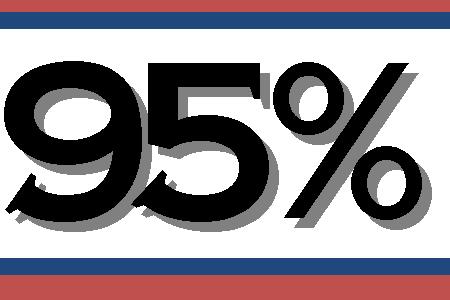
Percentage of EMS providers who reported having restrained patients.
* Facts according to a survey of 490 EMS providers in a Position Paper published by the National Association of EMS Physicians
Ambulances are regulated by various agencies throughout the country. However, in 27% of the states, no specific agency is responsible for ambulance regulations. For the safety of everyone involved, every organization should have a policy on how to deal with assaultive or agitated behavior in a patient. Regulated or not – you need to know how to keep yourself safe and then keep your patients safe. According to the recommendations in the Position Paper from naemsp.org, “The safety of EMS personnel is the paramount factor during PPR (pre-hospital patient restraint), followed by the importance of protecting patients from injuring themselves or others”.
Of course, you will want to know and understand your organization’s policy but, in general, most agree on these basic rules and principles to keep both EMS providers and their patients safe when it comes to combative, agitated or assaultive behavior.
8 Tips in Handling Agitated, Combative, Assaultive Patients
1. Consider the Source – Assaultive behavior may be caused by a psychiatric disorder but may also be a result of a medical condition such as:- Head Injury
- Drug or alcohol intoxication
- Metabolic disorders
- Hypoxia
- Dehydration
- Postictal state
3. Get the Facts - Obtain a detailed history from family members and information from law enforcement personnel and bystanders. Also make note of the patient’s surroundings for clues (such as medication or alcohol bottles, drug paraphernalia, etc.) as to the cause of this behavior.
4. Evaluate – According to the Best Practices in the Arrowhead Consulting Group Report - Psyciatric Patient Handling, Combative and non-combative presenting in medical transport (2):
“Pre-hospital patient restraint provides verbal, physical, and/or chemical restraint to allow for the safe transportation and treatment of the violent, combative, or agitated patient by EMS personnel. Properly applied PPR may reduce the possibility of patient injury, reduce the potential for injury to EMS providers, and allow for timely and appropriate treatment and transportation of a patient to a medical or psychiatric facility.”
Understand and refer to your organization’s policy in determining the need for restraints. Don’t hesitate to ask for or seek training. Do not be a part of the 72% who have not had any formal PPR training! Your safety and your patient’s safety is at stake.
5. Document the Process - When restraints are required, thoroughly document all facts including:
- patient assessment
- pertinent clinical information
- reason for restraint (and any evidence of factors leading to the patient’s level of consciousness or behavior)
- restraint procedure
- frequency of reassessment
- care during transportation
- documentation of monitoring restrained extremities
If applicable, when deciding to imply consent, also document facts contributing to the decision that patient was not competent.
6. Position Properly - Most policies reviewed include specific positioning requirements:
- Place patients in supine position, or in Fowler’s or semi-Fowler’s position.
- Patients should never be in a “hog-tied” or hobbled position, restrained in a prone position or be transported while sandwiched between back boards or mattresses.
- Restraint should never compromise the airway or constrict the neck and should be able to be quickly removed if a patient develops respiratory distress or vomits.
- Restraints should not restrict the ability to easily turn the patient on their side and protect the patient’s airway should vomiting occur.
7. Monitor Frequently - Restraints must allow for frequent and regular monitoring of pulse and respiration. In addition, restrained extremities should be monitored and evaluated for circulation, sensory function and motor function in a frequent and regular manner – every 15 minutes is suggested.
8. Be Prepared - When things go wrong in transport:
-When an unrestrained patient becomes assaultive during transport, request law enforcement assistance. Be calm and try to calm the patient in a reassuring manner – remember, many of these issues result from fear or a fearful situation. Reassurance can calm the fear.
-If you believe your personal safety is at risk, do not inhibit the patient’s attempt to leave the ambulance (if moving, stop in a safe place). Make every effort to release the patient into a safe environment and stay on the scene until law enforcement arrives and controls the situation. Your safety comes first.
-There are devices available that can help to delay or deter the patients ability to undo their restrain buckles.
Learn more about Buckle Guard.
SUMMARY:
The best protocol is to understand and know your organization’s policy in dealing with combative or assaultive patients. These tips can address some of the basic principles and include some guidance on the agreed best practices to protect you and your patients; however, nothing can replace formal training consistent with your organization’s Pre-Hospital Patient Restraint policy. Your safety and your patient’s safety are of the upmost importance.
Want to read more? Here are a few of the resources we thought were helpful:
- Psychiatric Patient Handling -Combative and non-combative presenting in medical transport
http://www.arrowheadgrp.com/pdf/ambulance/Psychiatric_Patient_Transport_Handling.pdf - Contra Costa Emergency Medical Services: Managing Assaultive Behavior/Patient Restraint
http://cchealth.org/ems/pdf/policy30.pdf - Handle With Care: The Challenge of Transporting Suicidal Patients
http://www.jems.com/article/handlewithcare - Position Paper, National Association of EMS Physicians, “Patient Restraint in Emergency Medical Services Systems, Kupas, Douglas F., MD; Wydro, Gerald C. MD, February 28, 2002
http://www.naemsp.org/Documents/Position%20Papers/POSITION%20PatientRestraintinEMSSystems.pdf
This paper is brought to you by McNaughton Incorporated, Home of the Buckle Guard
Helping to Keep People Safely Buckled Up!
Minneapolis, MN, Made In USA, 800-423-5487, www.McIncDirect.com
For suggestions or comments on this article please email us at support@McIncDirect.com
**Please Note: These "8 Tips" are strictly based upon documented information and are in no way intended to replace formal, certified training or are intended to be any sort of formal training, policy or guide. Please seek formal training when needed.
For a Printer Friendly Version - Click Here

support@McIncDirect.com
Kitchen Organization Products | Window Vases | Television Wall Mounts
Child Car Seat Safety | Gift Wrapping Supplies | Unique Automotive Accessories
What's Hot! | Find A Retailer | Newsroom | About Us | Contact Us
Ordering Policies | Privacy Policy | Resource Center





